

Share
This story was originally published by ProPublica. ProPublica is a nonprofit newsroom that investigates abuses of power. Sign up to receive our biggest stories as soon as they’re published.
At the end of June, with hundreds of his workers already infected with COVID-19 and several dead, Kenneth Sullivan, the CEO of Smithfield Foods, the world’s largest pork producer, sent a pointed letter to two U.S. senators who had launched an investigation into outbreaks in meatpacking plants and industry warnings of an impending food shortage.
In blunt, unapologetic terms, Sullivan chastised critics for suggesting Smithfield had acted too slowly to prevent the disease from spreading among its workers and surrounding communities. These “revisionist historians,” he wrote, refused to be “bound to reality” by saying meatpackers could have spaced workers out, slowed processing lines or stockpiled face masks.
“What no one anticipated, and has never happened in our lifetimes, is the scenario we are living through today,” Sullivan wrote. “That is, our harvest facilities, which are the critical linchpin in the supply chain, could be threatened, en masse, by a global pandemic that threatens our ability to produce food.”
Sullivan’s sentiment has been echoed by meatpacking companies across the country: How could anyone have prepared for COVID-19?
But a ProPublica investigation has found that for more than a dozen years, critical businesses like meatpackers have been warned that a pandemic was coming. With eerie prescience, infectious disease experts and emergency planners had modeled scenarios in which a highly contagious virus would cause rampant absenteeism at processing plants, leading to food shortages and potential closures. The experts had repeatedly urged companies and government agencies to prepare for exactly the things that Smithfield’s CEO now claims were unrealistic.
“It was an unmitigated disaster for food processors, and it didn’t have to be,” said John Hoffman, who developed emergency planning for the food and agriculture sector at the Department of Homeland Security during the George W. Bush administration. “There are things that could have happened in a pandemic that would have been novel, but this has unfolded pretty much as the pandemic plan has suggested it would.”
Instead, the industry repeatedly expressed confidence in its ability to handle a pandemic, and when asked to plan, relied on a wait-and-see approach, records and interviews show.
“The bottom line is this: The world is in the midst of an unprecedented pandemic,” Keira Lombardo, Smithfield’s executive vice president for corporate affairs and compliance, said in a statement. “We challenge you to name anyone anywhere in the world who was entirely prepared for COVID-19.”
Nearly 15 years ago, the White House summoned the leaders of the food and agriculture industry, along with executives from other business sectors, to work with government officials to come up with a plan to sustain the nation’s critical services in a pandemic.
The Bush administration warned businesses that as many as 40% of their workers might be absent due to illness, quarantine or fear. Social distancing would be necessary in manufacturing plants, it said, even if it affected business operations. And government modeling showed that such high absenteeism would cut food production in half.
Industries should identify their critical workers and facilities now, DHS urged, and businesses should collaborate with their local public health agencies to prepare before a pandemic arrives.
Warnings of Absenteeism
Fourteen years ago, the federal government told businesses to prepare for large swaths of their staff to be absent.

Even then, the food sector’s task force underestimated the threat, telling the president’s infrastructure advisory council in 2007 that it had determined that “few, if any, critical food and agriculture facilities exist” that would warrant prioritization for a vaccine in the event of a pandemic.
When, and if, a pandemic arrived, its report said, the industry could rely on “American ingenuity” to “adapt and continue operating.”
In the years that followed, records show, government agencies and consultants tried to get the meat industry to participate in planning exercises. The industry’s trade association circulated a template for a pandemic plan that predicted “employee-to-employee disease transmission” would threaten operations. The Labor Department recommended that businesses with “high population density work environments” stockpile enough masks to provide each worker with two per day for 120 days. For a large meatpacking plant like Smithfield’s Sioux Falls, South Dakota, plant with 3,600 employees, that meant having 864,000 masks on hand.
Two Face Masks Per Employee Per Shift
Eleven years ago, the Labor Department encouraged employers to stockpile masks for “medium exposure risk” jobs that include those with “frequent, close contact (within 6 feet) exposures to other people such as co-workers” and the public.

Instead, most of the industry’s attention went to developing detailed protocols to prevent disease among poultry and livestock, viewed as a more likely threat.
“We were probably more prepared for animal pandemic issues than we were for human pandemics,” said one former meat industry executive.
By 2015, a federal report noted the food and agriculture sector still hadn’t identified which facilities were most crucial to maintain during any disaster, let alone a pandemic, and had “no overarching plan” for doing so. Several former managers at meatpacking companies told ProPublica they hadn’t gone through any pandemic planning other than reviewing general flu season recommendations in the years before 2020.
The United Food and Commercial Workers union, which represents workers responsible for the majority of U.S. beef and pork production, said it, too, was left out of the loop.
“If the packers did a lot of preplanning for this pandemic, I didn’t see it,” said Mark Lauritsen, the UFCW’s director of food processing, packing and manufacturing.
ProPublica contacted eight of the largest meat and poultry companies and none would answer specific questions about their pandemic planning before COVID-19. Some, like Smithfield, JBS and Perdue Farms, described in vague terms a variety of emergency planning. Tyson and Cargill had plans in the past but wouldn’t say whether they had been updated or tested. Hormel and National Beef didn’t respond to questions, and Sanderson Farms didn’t return calls or emails.
So, when COVID-19 outbreaks erupted in plants in March, the meatpacking companies were caught flat-footed, scrambling to install basic protections, such as plexiglass barriers between employees working side by side, and to find enough masks, reportedly causing workers at one Tyson plant in Waterloo, Iowa, to wear old T-shirts and sleep masks to cover their faces.
The companies’ lack of preparedness quickly overwhelmed tiny rural public health agencies, which found themselves fighting on the front lines of some of the world’s most intense hot spots. Hospitals from the Eastern Shore of Virginia to the High Plains of Colorado were flooded with sick workers and their family members, causing some doctors to fear they’d run out of ventilators.
With droves of workers absent, some plants suspended production. Supermarkets like Kroger and Costco limited the amount of meat customers could buy. Hundreds of Wendy’s fast-food restaurants ran out of hamburgers. Farmers euthanized millions of chickens and pigs. And beef, poultry and pork prices spiked, just as millions of people lost their jobs.
The meat industry’s struggles were compounded by President Donald Trump’s early dismissal of the virus, his administration’s slow and poorly coordinated response and shifting guidance from the Centers for Disease Control and Prevention.
The federal agencies with oversight over the industry did little to help. The Labor Department had pandemic guidance for businesses that it had created back in 2007. But it didn’t release updated guidance for COVID-19 until the second week of March, after cases began popping up in workplaces, and didn’t issue specific guidance to meatpackers until the end of April.
The U.S. Department of Agriculture had relaxed its vigilance on human pandemic planning in recent years and failed to help plants prepare in the early days of COVID-19, emergency planners and former federal officials said.
It wasn’t until the end of April, after 5,000 workers had been infected and dozens killed, that most of the major meatpackers implemented policies that had been called for more than a decade before. Today, more than 39,000 meat and poultry workers have tested positive for COVID-19, and at least 170 have died, ProPublica has found.
So when Smithfield and Tyson raised the alarm that the nation’s meat supply chain was in danger, it came as little surprise to many of the country’s infectious disease experts and emergency planners.
They had been predicting it would break for years.
“I’ve heard it a thousand times in the last six months: ‘My, this has taken us all by surprise,’” said Michael Osterholm, director of the Center for Infectious Disease Research and Policy at the University of Minnesota. “I’ve written for the last 20 years about exactly what’s happening today.”
In 2004, a strain of avian flu jumped from birds to humans, and dozens of people in Asia got sick and even died from the disease. To policymakers and infectious disease experts, this was a worrisome sign that the next global outbreak was imminent. Pandemics became a priority around the world, and in November 2005, the White House issued a National Strategy for Pandemic Influenza.
For the next several years, federal pandemic planning proceeded at an urgent clip. In spring 2006, the federal government issued a 233-page implementation plan that laid out how the government would protect everything from human and animal health to public safety in the face of an outbreak. And it dedicated a chapter to safeguarding 17 components of the nation’s critical infrastructure, including dams, power lines and the food supply.
The plan had an flu outbreak in mind, but much of the thinking has been applicable to COVID-19, emergency planners said. It assumed that there would be asymptomatic carriers and that vaccines and antivirals wouldn’t be immediately available. It also recommended infection control measures like social distancing, increased sanitation and frequent hand-washing.
Schools and some businesses might need to close to blunt transmission. Meanwhile, essential enterprises needed to plan for ways to run their operations while limiting the disease’s spread and preparing for as many as 40% of their employees becoming unavailable.
DHS issued an 84-page guide for those businesses on how to prepare for a pandemic and what to expect from the government when an outbreak occurs. It asked them to think through, for example, how they could find dedicated transportation for workers, stagger break times and modify workspaces in offices and plants to allow for social distancing.
In spring 2007, the U.S. Health and Human Services Department issued interim guidance that said people should consider wearing masks during a pandemic if they needed to be in a crowded place.
In 2009, the Labor Department issued guidance encouraging businesses to stockpile masks if their employees worked close together. But Smithfield, JBS and Perdue told ProPublica they hadn’t stockpiled any masks before the coronavirus. Tyson said it had purchased additional personal protective equipment, or PPE, to outfit response teams during the 2015 avian flu outbreak, but for COVID-19, it “would not meet the needs of even one plant location for one day.”
Instead, as the outbreaks began, JBS handed out balaclavas to its workers in Greeley, Colorado. Tyson eventually chartered a cargo plane to China to obtain masks.
“If we truly learned the lessons and stockpiled, then we might have been in a better place, but that’s an economic commitment that companies that are operating on narrow margins may not want to make,” said David Acheson, who was in charge of food defense and emergency response at the FDA during the Bush administration.
Balaclavas Instead of Masks
A Centers for Disease Control and Prevention team found workers at a JBS plant in Greeley, Colorado, wearing insufficient face coverings.

As the nation’s pandemic planning proceeded, DHS assigned researchers at the Sandia and Los Alamos national laboratories to model what could happen during an outbreak. The researchers presented simulations that showed a peak absentee rate of 28% and noted that if the rate remained above 10% for several weeks, it would cut food production in half. Approximately 40% of firms would “cease operations due to insufficient levels of labor,” researchers said.
“The main takeaway is that if enough people are missing from work at these plants for long enough, you can get disruptions of food,” said Mark Ehlen, a Sandia research scientist who worked on the study.
The prediction has been uncannily accurate. Documents obtained by ProPublica through public records laws show that from North Carolina to Kansas to Nebraska, meatpacking plants experienced up to 50% absenteeism on processing lines, which led cattle slaughter to fall by 40% and pork production by more than half at the end of April. Then, Trump invoked the Defense Production Act to help keep plants running, which pressured state and local health agencies to back away from their recommendations to temporarily close them to get the disease under control.
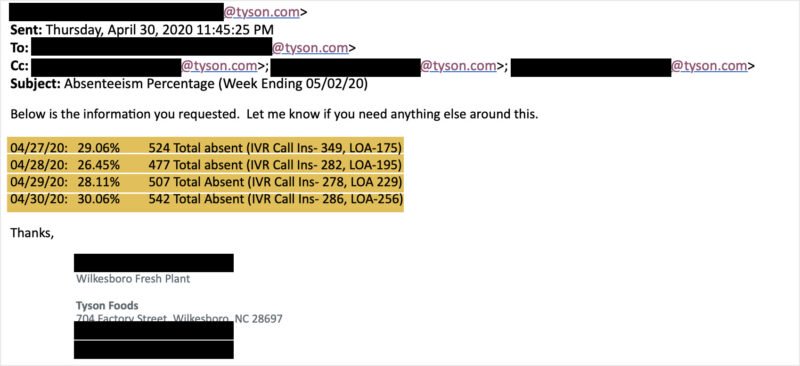
Hundreds Out Sick at a Tyson Plant
Absenteeism reported by a Tyson human resources manager reflected predictions of labor shortages.
Since the earliest days of pandemic planning, the federal government knew it needed buy-in from businesses since the vast majority of critical infrastructure is owned and operated by the private sector. So in 2006, then-HHS Secretary Michael Leavitt took his message on the road.
“Our message was very clear: A pandemic is coming, and if you believe that somehow the federal government will ride to your rescue, you will be tragically mistaken,” Leavitt said in an interview. “Not because we lack the will or the wallet but because a pandemic is different than any other kind of emergency and it requires a planning ethic across society — states, government, schools, hospitals, families and businesses.”
DHS had already created a group to get business owners and CEOs talking to government officials about disaster preparedness and response. The Critical Infrastructure Partnership Advisory Council often discussed threats like hurricanes and cybersecurity, but in 2007, pandemic flu made the agenda.
In the food and agriculture sector of the council, the heavy lifting has often fallen on Clay Detlefsen, who works for a dairy industry association. Detlefsen had created a pandemic plan in 2006 for the dairy industry, which he adapted for the food and agriculture sector in 2007. The North American Meat Institute made it available online soon afterward.
That year, a White House infrastructure advisory group reported on which essential workers should be prioritized for a vaccine during an outbreak. The section from the food and agriculture representatives was short on specifics. Though parts of the industry, like meatpacking, are deeply consolidated, it said the sheer number of businesses made it essentially pandemic-proof.
Trade associations reiterated the message after President Barack Obama’s election, when the USDA brought them together for a tabletop exercise called “Flu for Thought II.” The scenario envisioned an outbreak that would lead to a shortage of food safety inspectors, requiring some plants to close.
Caroline Smith DeWaal, who attended the exercise as food safety director for the Center for Science in the Public Interest, said that when she asked about potential food shortages, she remembers being told, “Don’t worry, other parts of the country will supply the food.”
When emergency planner Regina Phelps looked around in 2007, she was worried: Despite the drumbeat of warnings, many companies weren’t acting fast enough to prepare for a pandemic or, worse, were becoming complacent. Phelps had been doing disaster consulting for multinational companies since 1982, and it was her job to think about worst-case scenarios and translate government guidance for businesses.
Maybe, Phelps thought, if she could make them feel the toll a pandemic could take, they would do something. So, she convinced Roche, the maker of Tamiflu, to sponsor a series of tabletop exercises for executives in different industries.
While many food companies, including Smithfield and Tyson, declined her invitation, Phelps said, some of the nation’s biggest meat buyers accepted. In February 2008, at the Michelangelo Hotel in midtown Manhattan, executives from PepsiCo, Sysco, Nestlé, Food Lion, Compass Group and Target discussed how a pandemic would unfold in the food industry.
A pandemic would last far longer than other kinds of disasters and affect every worksite, Phelps warned them. A relationship with the local public health department would be critical because “by invoking public health law, it can essentially control the destiny of your organization,” she wrote in a detailed report after the event.
At one point, the conversation turned to perhaps the most critical question the meat industry has faced in COVID-19: How would workers “social distance” on a food processing line?
“They really couldn’t come up with a clear, comfortable answer,” Phelps recalled in an interview. “The answer would be: ‘Well, that would really impact production.’ ‘Are you willing to do that?’ ‘Well, I don’t know. We’d really have to see how bad it was.’”
Workers Unable to Distance in a Cafeteria
A photo shows people crowded in the cafeteria of a JBS plant in Plainview, Michigan, in late April, unable to socially distance despite an outbreak at the plant.

Without the ability to social distance, Phelps wrote, having masks might make the difference between being open or closed. “One participant expressed the fear of many,” the report noted, “when he said, ‘What scares me is that we’re not going to have enough antivirals or masks when we need them if we don’t get them now.’”
When COVID-19 hit, Phelps said, it was those companies that had prepared, particularly financial institutions, that not only had masks but were able to donate them to hospitals in need.
“All of the things that have occurred, we had all predicted,” she said. “People just can’t believe it’s going to happen to them.”
The first real-world opportunity to test this rush of pandemic planning came in 2009 with H1N1, also known as swine flu, which originated in central Mexico.
Some meatpackers drew on their pandemic planning and took precautions at their facilities. According to news reports, ConAgra distributed masks to workers at its popcorn and ketchup plant in Mexico and stationed a doctor there. Cargill restricted travel to its Mexico operations and instructed local managers to revisit their crisis management plans to figure out how they could continue operations amid an outbreak.
Meanwhile, Tyson said in its 2009 sustainability report that some of its employees had contracted H1N1, but that it had communicated to employees how to protect themselves and their families.
In a webinar that September, as the government braced for a second wave, the USDA’s Food Safety and Inspection Service urged the meat industry to remain alert. In closing, USDA official Perfecto Santiago offered a poignant warning about complacency.
“Because the pandemic has been mild,” he said, “we might tend to put the pandemic plan somewhere that it will probably gather a few pieces of dust. Let’s not get into a rut. Let’s review the plan. Let’s update them, and let’s test them.”
But in the years that followed, Santiago’s warning would go largely unheeded.
“There’s nothing worse than having a disaster when it’s not that bad,” Phelps said, “because people think: ‘We didn’t need to do all this. We did fine.’”
Between 2000 and 2009, Phelps said, she wrote about 500 pandemic plans for companies. Between 2010 and 2019, the number dropped to about 20.
The food and agriculture industry had also become less engaged in the DHS critical infrastructure council around the time that H1N1 came and went. Detlefsen said that while there was interest in participating in the group after 9/11, energy and attendance from industry faded over time. The diversity of industries — from farms and meat processors to restaurants and grocery stores — made conversations about priorities difficult, he said. Many businesses, located outside Washington, saw the threats as theoretical and unlikely.
One meat industry executive described the meetings as “another one of those trade association things.”
“I accept the reality and don’t put blame on anyone,” said Detlefsen, who has remained volunteer co-chair of the council for nearly two decades as others have stepped away. “Everyone has their challenges and priorities.”
A membership roster from 2010 showed the group had become stacked with trade associations, and not a single meatpacking company was listed.
“We didn’t have that many CEOs,” said R. James Caverly, who ran DHS’ public-private partnership in critical infrastructure from 2003 to 2013. “A trade association, at the end of the day, they can’t direct people to do something, and they don’t make investment decisions.”
After H1N1, he added, “pandemic planning meant there was a book somewhere on the shelf, and other more pressing issues took precedence.”
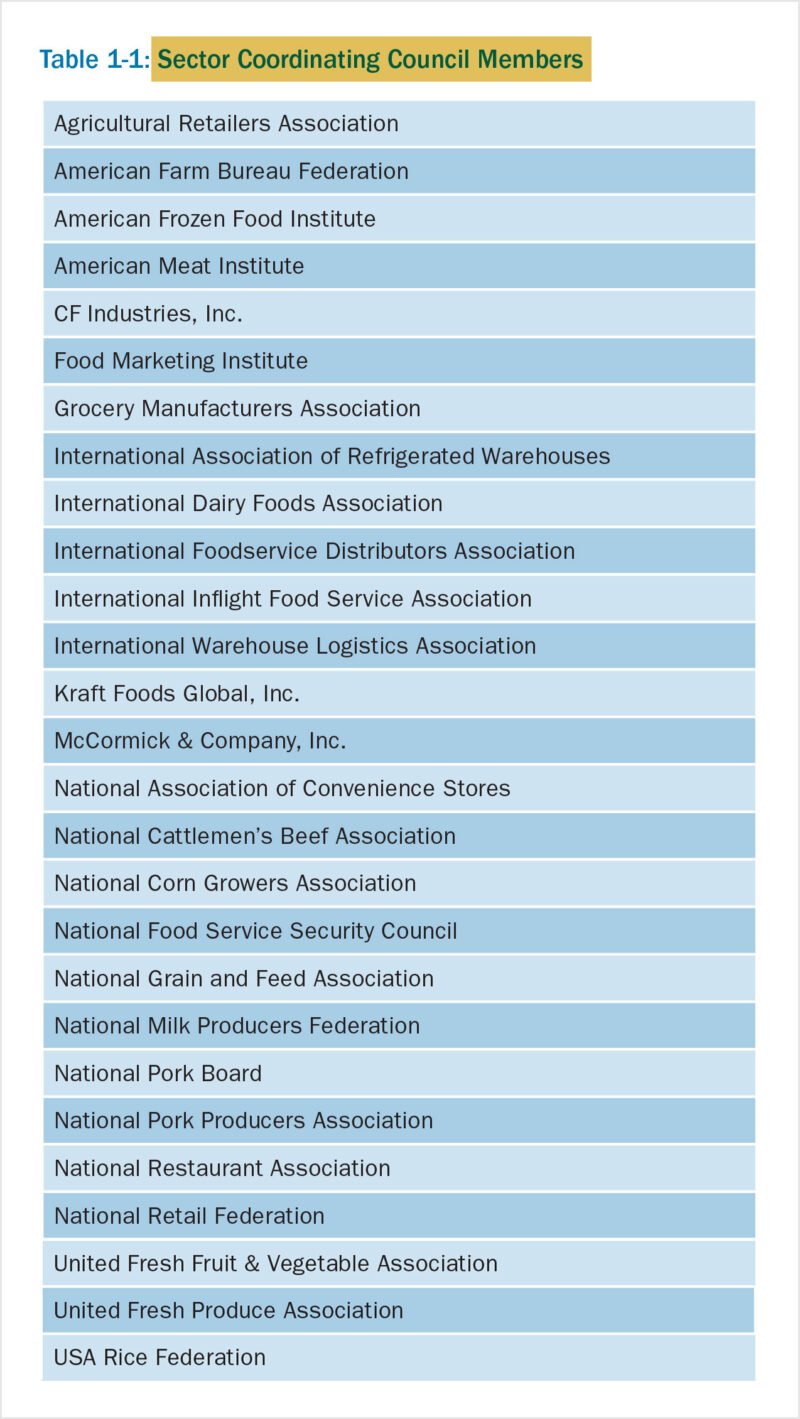
Trade Associations but No Meatpacking Companies
In 2010, participants in Department of Homeland Security disaster planning for the food and agriculture sector tilted toward trade groups.
The food and agriculture sector’s 2010 contribution to the National Infrastructure Protection Plan mentions a pandemic only twice in passing. Attention had turned to animal diseases, foodborne illnesses and the intentional contamination of the food supply. The government and industry continued to run tabletop drills for those emergencies, but dozens of officials interviewed for this story couldn’t remember any that related to a human pandemic.
Caitlin Durkovich, assistant DHS secretary for infrastructure from 2012 to 2017, said by then, cybersecurity and the rise of the Islamic State had diverted a lot of attention. “It’s hard to blame the food and ag sector writ large,” Durkovich said. “There was just a systemic failure across government to keep its eye on this threat.”
Some researchers have tried to revive the attention to pandemics and the risk they posed to the food supply.
Andrew Huff, a former Sandia researcher, noticed the food industry had become increasingly consolidated after H1N1 and created a model that showed “significant and widespread food shortages.”
In 2014 and 2015, he tried to raise this issue with policymakers whenever he visited Washington. Ebola was ravaging West Africa and bird flu was circulating again, bringing infectious disease concerns back to the foreground. But Huff said little came of his visits. “A lot of times, they say, ‘Good job,’ and they do not do anything,” he said. “No one had any political will to do anything about it.”
Under the Obama administration, the federal government had put its money and political interests into the Global Health Security Agenda, which shifted attention to controlling outbreaks abroad and away from planning for them in the United States, said Joseph Annelli, a former USDA official who worked on pandemic planning for the Bush administration.
But as recently as last year, researchers continued to lay out the challenges American meatpacking plants would face during an outbreak. In 2019, Chia-ping Su, a Taiwanese infectious disease expert who did a fellowship at the CDC, published a paper stressing the importance of workplaces in controlling infectious diseases.
Working with others at the CDC’s occupational safety institute, Su highlighted numerous issues that would come to hinder the COVID-19 response. One incident, a 2011 tuberculosis outbreak at a meatpacking plant in Amarillo, Texas, showed how carpooling could be a source of infection and how multiple language barriers and fears of retaliation could challenge an investigation.
“As a worker, you spend more than eight hours in your workplace, probably more than the time you spend in your house with your family,” Su said in a Skype interview from Taiwan. “So, if you talk about infectious disease prevention or control, it’s very important to focus on the workplace.”
But in the United States, he noted, the health system rarely records industry or occupation when sending lab results to public health agencies and the CDC. This has been a particular problem with COVID-19, delaying epidemiologists’ ability to recognize workplace-related outbreaks, public health officials said.
In retrospect, they said, the nature of work in meatpacking plants made them obvious hot spots.
“You put 3,000 people in a meatpacking plant after it’s been declared a human transmissible disease,” said Robert Harrison, director of University of California, San Francisco’s occupational health program. “It doesn’t take a rocket scientist to know you have to implement prevention programs. This is the most disastrous and eminently preventable occupational disease in my career as an occupational medicine doctor.”
In February, John Hoffman, a senior research fellow with the University of Minnesota’s Food Protection and Defense Institute, started “ringing the bell hard” about an impending pandemic. Hoffman, who advises DHS on the food and agriculture sector, said he began calling his contacts in civil service, academia and industry — including meat and poultry — to ask them why they weren’t activating the national pandemic plan. (Hoffman stressed he was not speaking on behalf of the University of Minnesota or DHS.)
To help the food and agriculture sector prepare, for example, he thought USDA inspectors could easily work with plant managers to figure out infection control strategies.
But, he said, his urgency wasn’t widely shared. In March, Hoffman circulated a document among government officials that outlined key portions of the Bush-era pandemic planning related to critical infrastructure. With evident frustration, he wrote that time for the two initial phases of pandemic response — planning and preparation — had been lost because of “erroneous guidance” from the CDC and “delays in decisions and lack of cross infrastructure coordination” by the government. As a result, industries like agriculture and food found themselves immediately in the response phase. By then, he wrote, companies had lost the chance to obtain PPE and to work with local and state government on issues like infection control “until the level of sick employees became critical and the operational viability came into question.”
His outreach was met with silence, resistance or even ridicule from some agencies and industry representatives, he said. “I was called an ‘old lunatic,’” he said. “That’s the environment. It’s nuts. It’s not professional.”
Failing to follow the national guidance developed 15 years ago led to the breakdown at the meatpacking plants, Hoffman said. The government deserves the lion’s share of blame because it didn’t follow the pandemic plan, he said, and failed to provide leadership to the industry. “When government didn’t step up,” Hoffman said, “the companies were left to their own devices.”
Tyson representatives said the company formed a coronavirus task force in January to assess risks and begin working on mitigation plans and sourcing PPE. But on the ground, there was chaos. “Suffice it to say that whatever pandemic plan they had wasn’t adequate,” said a former Tyson supervisor. “Everyone was scrambling.”
JBS, which has dozens of beef, pork and chicken plants in 26 states, said it began holding daily planning meetings with executives in February to track CDC guidance. But a former JBS supervisor told ProPublica that the company didn’t start its COVID-19 response at its plants until March, and while he was aware of emergency plans for fires, hurricanes and tornadoes, “I don’t remember ever talking about a pandemic,” said the employee.
Detlefsen said he also tried to get pandemic plans in front of the food and agriculture industry in early March. An official with the FDA got in touch and said, “We ought to dust off the continuity of operation plans and get that out into the food and agriculture sector entities in case this goes bad,” he recalled. “And then bam, within a week or 10 days, everything was hitting the fan.”
When the FDA reached out again later that month, Detlefsen said he told the agency: “If they didn’t have a plan in place, it’s too late already.”
Despite warnings about the need to establish relationships with local public health officials, emails from multiple states show that Tyson didn’t begin contacting local health agencies about COVID-19 until mid- to late March. Many other companies didn’t reach out at all — or like Smithfield failed to respond to some health officials’ inquiries.
Officials in Crawford County, Iowa, struggled for a month to reach anyone from Smithfield about the company’s efforts to prevent COVID-19 at its pork plant there. In increasingly frustrated emails, Kim Fineran, the county public health director, said she’d enlisted the mayor of Denison, the chamber of commerce, a state representative, the local union and the state Health Department, but Smithfield seemed to ignore all of them.
“We’re likely to have an explosion of cases in Crawford and surrounding counties if we don’t get a handle on this,” Fineran wrote in an email on March 31. “We cannot impact the business if they won’t respond to us.”
After a spike in May, Crawford has the second-highest cumulative infection rate of Iowa’s 99 counties. But neither the company nor state officials have released how many cases are tied to Smithfield.
A Smithfield spokesperson said the company has been “in frequent communication with a host of local, state and federal health authorities” during the pandemic.
“I Have No Access to Any Information About These Cases”
Kim Fineran, the public health director for Iowa’s Crawford County, warned in an email that the Smithfield plant’s failure to share information posed a threat to the community.

The first contact Lauritsen of the UFCW had with a meatpacking company about the coronavirus was in mid- to late February, he said, when he called an employer to ask about the plan if a worker needed to be quarantined. That led to discussions with most of the big meatpackers about eliminating waiting periods for short-term disability, extra pay and expanded paid leave.
When the pandemic hit, some meatpackers announced adjustments to their leave policy to protect older workers and encourage sick ones to stay home. Despite benevolent messages from the meatpackers’ corporate leadership, public health departments across the country received numerous complaints that supervisors were telling workers to come back to work while still symptomatic and threatening to fire them if they didn’t.
Many workers said they feared calling in sick, regardless of any new policies, given the industry’s long-standing policy of penalizing those who did so.
“With very abrasive attendance requirements prior to COVID, I fear that they are well groomed to the expectation of working when ill to avoid punitive retaliation,” Gina Uhing, the director of a Nebraska health district that’s home to a Tyson plant, observed in a mid-April email.
At a JBS plant in Michigan, a state epidemiologist in April documented 13 cases in which employees continued working despite experiencing fevers and other symptoms. An occupational health nurse at the plant wrote to the county Health Department that “even someone in management was threatened with their job.” She “feels like upper management is not taking this seriously, and not communicating with employees,” according to notes from the call.
In his letter to members of Congress, Smithfield’s CEO bristled at the criticism that it had acted too late. But in an April 12 email to Colorado health officials, South Dakota’s state epidemiologist, Josh Clayton, who’d been investigating a major outbreak at the company’s Sioux Falls plant, wrote, “Smithfield Foods was initially slow to increase their precautions.”
The CEO’s letter was signed by more than 3,500 Smithfield employees — mostly white-collar workers and managers. It included virtually no one on a processing line, where the virus raged.
Dulce Castañeda, whose father works at the Smithfield plant in Crete, Nebraska, said her father watched his co-workers, including someone next to him, get sick. She said the lack of front-line workers signing the letter is notable.
Someone should ask those workers, she said, or their families, who may have been exposed to COVID-19 through them, whether the senators’ criticism of Smithfield was valid.
To claim no one should criticize the company, she said, “implies they are above the law, above critique, above everything.”
Mollie Simon contributed reporting.

